Authors: Samantha Hunt, Jonathan Boulton, Tim Slade / Editor: Liz Herrieven / Reviewer: Tim Slade / Code: / Published: 31/12/2019 / Reviewed: 31/03/2026
Eyes are the windows to the soul. They have the power to mesmerise and enchant even the hardest of hearts. Yet, for many clinicians, they also instil genuine fear. Ophthalmology is a specialist area with very limited undergraduate exposure, even though sight is highly valued by patients, who rate blindness worse than loss of hearing or of a limb. The RCEM curriculum tells us that EM clinicians are expected to be able to manage red and/or painful eyes, sudden vision loss and facial trauma. Thankfully, the majority of eye conditions we see are not immediately sight-threatening, but what happens on the rare occasions when they are?
One such rare emergency is orbital compartment syndrome. This is usually caused by retro-bulbar haemorrhage or orbital cellulitis. The rising pressure results in ischaemia to the sensitive neurological tissues of the optic nerve and retina and can be devastating to sight. Traditional understanding suggests that irreversible profound sight loss occurs within about 100 minutes of onset of ischaemia, although more recent data suggests this is more likely to be 12-15 minutes. Therefore, early recognition and intervention are vital to optimising visual outcome. Treatment should not be delayed waiting for radiological confirmation of a clinical diagnosis, or for a non-resident ophthalmologist.
Recognition of orbital compartment syndrome
Orbital compartment syndrome is a clinical diagnosis recognised by a collection of signs and symptoms with a relevant risk factor such as facial trauma, a coagulation disorder or recent infection. These may not all be present, so a high index of suspicion is required.
Symptoms may include:
- Severe eye pain
- Profound vision loss
- Diplopia
Signs may include:
- Proptosis
- Restricted eye movements
- Poor visual acuity
- High intraocular pressure (which can be assessed using digital pressure and comparison with the unaffected, or your own eye, if you dont have access to tonometry)
- Subconjunctival haemorrhage
- Swollen and bruised lids
- Relative afferent pupillary defect
The most important features to recognise are likely: relative proptosis, eyelids that are difficult to open with finger pressure, and presence of a RAPD in the traumatised eye.
Orbital compartment syndrome can also rarely be caused secondary to sinusitis, but this is a rare presentation and management differs subtly. Consultation with ENT and Ophthalmology should be considered prior to proceeding as management is often surgical rather than need for ED lateral canthotomy.
Video courtesy of the authors

Image 1 – Courtesy of the authors
Note fullness of the left upper lid denoting proptosis (this patient has already had canthotomy/cantholysis), with bruised lids and subconjunctival haemorrhage.
Management of orbital compartment syndrome:
If orbital compartment syndrome is likely, remember “Time is Vision“. An intervention should occur at the earliest possible opportunity. Lateral canthotomy and cantholysis is a quick and safe procedure with minimal risks to the patient and huge potential benefits. The only contraindication would be an open globe, which would warrant discussion with ophthalmology.
A survey of EM doctors in the United Kingdom published in 2019 identified that just 37% would be willing to undertake this procedure, with 91% citing lack of training. It is hoped this learning resource alongside the practical procedures SLO in the 2024 RCEM curriculum will have improved this situation EM3 created Resus Drills packs to improve training on this issue, and between February and September 2019, these have been viewed about 12,000 times. Traditionally taught using textbooks or cadavers, there are now a variety of low-cost simulation models to train for this rarely-undertaken but sight-saving procedure – two examples are here and here. Whilst simulations have limitations, they provide a good visual and kinetic way to learn a skill encountered rarely in clinical practice.
Step-by-step guide to lateral canthotomy and cantholysis:
We advocate the use of a Local Safety Standards for Invasive Procedures (LocSSIP) for ED practical procedures especially HALO procedures such as lateral canthotomy and cantholysis. An example from plymouth can be found here.
1. Obtain verbal consent
2. Local anaesthetic infiltration – superficially to skin +/- deep to orbital rim. Using one with adrenaline in, if readily available, will help with haemostasis. In addition, consider using Proxymetacaine or other local anaesthetic eye drops. Sedation should also be considered if appropriate.
Image 2 – Courtesy of Richard Ceaser Surgery
3. Use artery clamp on tissues between the lateral canthus and orbital rim to improve haemostasis.
4. Initial skin incision – (this can be combined with canthotomy in one go by using a pair of scissors if easier) – extend as far as orbital rim only (approximately at the end of the patients eyebrow if difficult to feel the rim)
5. Canthotomy – cut through the lateral canthus (where upper and lower lid meet) and tendon, all the way to the orbital rim using scissors. LIFT THE SHARP EDGES UP AWAY FROM THE GLOBE.

Image 3 – Courtesy of Richard Ceaser Surgery
6. Inferior cantholysis – free the lower lid by strumming the inferior canthal tendon and cutting through it with scissors (this can also be done on the upper lid if necessary)
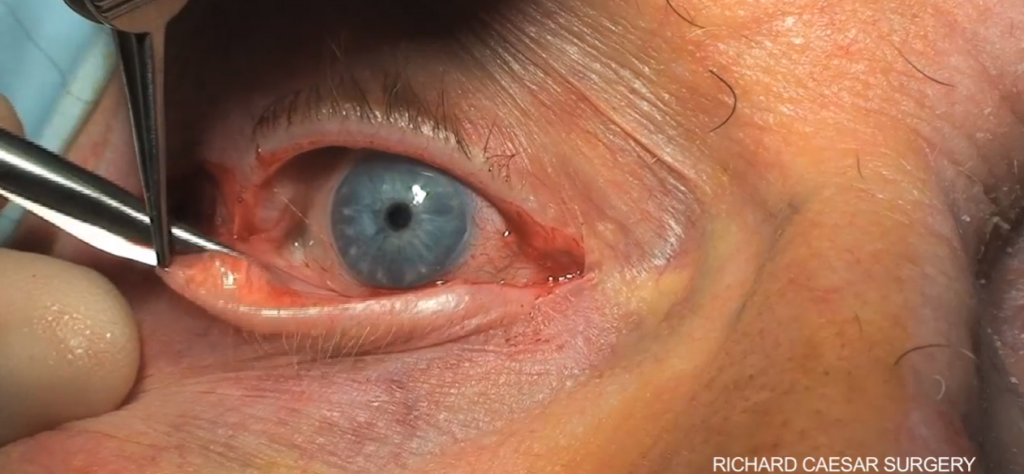
Image 4 – Courtesy of Richard Ceaser Surgery
7. Freely swinging lid (upper lid is being held up with a finger here)

Image 5 – Courtesy of Richard Ceaser Surgery

Image 6 – Courtesy of the authors

Image 7 – Courtesy of the authors
A free-swinging lower lid post-emergency canthotomy/inferior cantholysis
The endpoint:
When undertaking cantholysis of the inferior crus, how do you know whether you have done enough, or whether you need to also undertake cantholysis of the superior crus? Blood may be seen escaping from the orbit, the patient may report reduced pain and improved vision, their pupil may begin to respond more appropriately to light stimuli, and the intraocular pressure may improve. It is a simple procedure for an oculoplastic surgeon to repair the eyelids following cantholysis once the underlying aetiology has resolved. As such, if there is any doubt as to whether an inferior cantholysis is adequate, it is safest to also proceed to superior cantholysis. [Editor: I was once told by a friendly ophthalmologist that You won’t make any mess that we can’t fix]
Some have recently advocated a one snip technique, [TS1] however, the authors do not advocate this, as it is felt to have an increased risk of failure to decompress, damage to the tarsal plate with potential associated deformity, damage to rectus muscle and for superior canthus damage to the lacrimal ducts. These risks are felt to be increased compared to the normal practice of lateral canthotomy and cantholysis due to the more medial position of the incision.
Summary and learning points:
- Orbital compartment syndrome is a rare but sight threatening problem.
- Orbital compartment syndrome is recognised through symptoms and signs: proptosis, restricted eye movements, severe pain, vision loss, relative afferent pupillary defect and high intraocular pressure.
- If orbital compartment syndrome is suspected, time is vision.
- Lateral canthotomy and cantholysis is a quick, straightforward, low-risk procedure that aims to release the pressure on the optic nerve and retina, reducing ischaemic injury and the subsequent risk of permanent sight loss.
- If in doubt, do it. If in doubt, do more!
References and Further Reading:
-
- RCEMLearning podcast – lateral canthotomy. 2019.
- RCEMLearning Reference – Zygomatic Complex and Nasal Injury. Reviewed in 2025.
- Davies F. Resus drills #1: lateral canthotomy (v1.1. EM3, 2023.
- RCEM Curriculum 2021 Skills Resources-SLO6.
- Scott AW, et al. Public Attitudes About Eye and Vision Health. JAMA Ophthalmol. 2016 Oct 1;134(10):1111-1118.
- Hayreh SS, Weingeist TA. Experimental occlusion of the central artery of the retina. IV: Retinal tolerance time to acute ischaemia. Br J Ophthalmol. 1980 Nov;64(11):818-25.
- Tobalem S, Schutz JS, Chronopoulos A. Central retinal artery occlusion – rethinking retinal survival time. BMC Ophthalmol. 2018 Apr 18;18(1):101.
- McInnes G, Howes DW. Lateral canthotomy and cantholysis: a simple, vision-saving procedure. CJEM. 2002 Jan;4(1):49-52.
- Edmunds MR, et al. Management of acute retrobulbar haemorrhage: a survey of non-ophthalmic emergency department physicians. Emerg Med J. 2019 Apr;36(4):245-247.
- Nadir N, et al. The Halloween Lateral Canthotomy Model. 2017.
- Kong R, Kaya DP, Cioe-Pena E, Greenstein J. A low fidelity eye model for lateral canthotomy training. Afr J Emerg Med. 2018 Sep;8(3):118-122.

